Digestive and Immune Disorders: How Gut Health Affects the Whole Body
Key takeaways
- The digestive system and immune system are closely interconnected, with much of the immune system located in the gut.
- The gut microbiome plays a major role in regulating inflammation, metabolism, and immune responses.
- Disruptions in gut health can contribute to digestive disorders, autoimmune diseases, and chronic inflammation.
- Gut health influences many body systems including the brain, skin, metabolism, and immune defense.
- Understanding digestive–immune connections helps explain why chronic diseases often involve multiple body systems.
The digestive system does far more than simply break down food. Inside the gastrointestinal tract lives a vast ecosystem of microorganisms—collectively called the gut microbiome—that interacts closely with the immune system, metabolism, brain function, and inflammation pathways throughout the body.
The Gut as a Central Hub for Health
The digestive tract is one of the body’s most complex and active biological systems. Beyond digesting nutrients, it acts as a major interface between the external environment and the body’s internal systems.
- Physical barriers such as intestinal lining cells
- Immune defenses embedded within the gut wall
- Beneficial bacteria that help regulate harmful microbes
The Gut Microbiome: Your Internal Ecosystem
Trillions of microorganisms live within the digestive tract. This diverse microbial community—known as the gut microbiome—includes bacteria, viruses, fungi, and other microbes.
A healthy microbiome performs several critical functions:
Supporting Digestion
Certain gut bacteria help break down complex carbohydrates and fiber that the human body cannot digest on its own. In doing so, they produce short-chain fatty acids, which help nourish intestinal cells and support metabolic health.
Regulating Immune Function
A large portion of the immune system is located in gut-associated lymphoid tissue (GALT). Gut microbes interact with immune cells, helping the body distinguish between harmful pathogens and harmless substances.Maintaining the Gut Barrier
Beneficial microbes support the intestinal lining, which acts as a selective barrier. This barrier allows nutrients to pass into the bloodstream while preventing harmful bacteria and toxins from entering circulation.Disruptions to the microbiome—often called dysbiosis—can weaken these protective mechanisms.
The Gut–Immune System Connection
Approximately 70% of the body’s immune cells reside in the gut. This makes the digestive tract one of the immune system’s most active regulatory centers.
- tolerate it (such as food proteins and beneficial microbes), or
- mount a defensive response (against pathogens).
Digestive Disorders Linked to Gut Health
When gut function becomes impaired, digestive symptoms are often the first sign. These disorders can arise from inflammation, microbial imbalance, or disruptions to intestinal motility.Common digestive conditions linked to gut dysfunction include:
Irritable Bowel Syndrome (IBS)
IBS is characterized by abdominal pain, bloating, and changes in bowel habits. Research suggests that gut microbiome changes and altered gut–brain signaling may contribute to symptoms.Inflammatory Bowel Disease (IBD)
Conditions such as Crohn’s disease and ulcerative colitis involve chronic inflammation of the digestive tract. These diseases often involve complex interactions between genetics, immune responses, and the microbiome.Food Sensitivities and Intolerances
Digestive discomfort after certain foods may result from microbial imbalances, impaired enzyme activity, or immune reactions to food proteins.How Gut Health Influences the Whole Body
Gut health does not operate in isolation. Instead, it interacts with many systems throughout the body.Brain and Nervous System
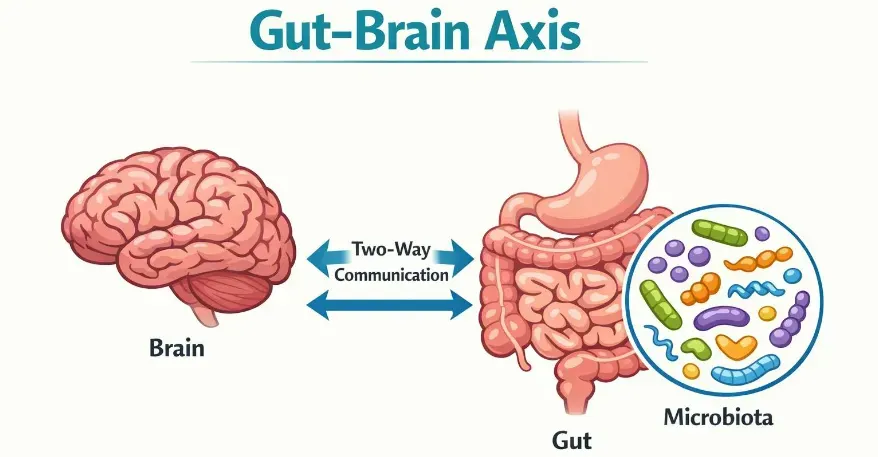
The gut–brain axis describes communication between the digestive system and the brain. Gut microbes produce neurotransmitters and signaling molecules that influence mood, cognition, and stress responses.
Immune and Autoimmune Conditions
Dysregulation in gut immune activity may contribute to autoimmune diseases in which the immune system mistakenly attacks healthy tissues.Metabolic Health
The microbiome plays a role in regulating metabolism, insulin sensitivity, and energy balance. Alterations in gut bacteria have been linked to obesity and metabolic disorders.Skin Health
Inflammatory skin conditions, including eczema and psoriasis, may be influenced by immune signals originating in the gut.Inflammation: The Common Thread
Many chronic illnesses share one underlying feature: persistent low-grade inflammation.
- joints
- metabolic function
- cardiovascular health
- neurological systems
Factors That Influence Gut and Immune Health
Many lifestyle and environmental factors can affect the balance between digestive and immune systems.Common influences include:
Diet
Diet strongly shapes the microbiome. Fiber-rich foods, fermented foods, and diverse plant nutrients tend to support microbial diversity.Antibiotics and Medications
Antibiotics can significantly alter gut bacteria by eliminating both harmful and beneficial microbes. Some medications may also affect microbial balance.Stress
Chronic stress can influence gut motility, microbial composition, and immune signaling through the gut–brain axis.Sleep and Circadian Rhythm
The microbiome follows daily cycles influenced by sleep patterns and meal timing.Early-Life Microbial Exposure
Early exposures—such as birth method, breastfeeding, and early diet—help shape the developing microbiome and immune system.Why Understanding Digestive–Immune Connections Matters
Digestive and immune systems work together to maintain internal stability. When the balance between microbes, immune responses, and intestinal barriers remains healthy, the body can effectively manage inflammation and defend against disease.This growing understanding has changed how researchers view chronic disease. Rather than focusing on isolated organs, scientists increasingly recognize the importance of system-wide interactions, with the gut acting as a central hub.
Related Articles:
- Gut Health and Chronic Disease: What’s the Connection?
- Autoimmune Conditions Explained Simply
- IBS and Digestive Disorders: Symptoms and Triggers
- How Immune Dysregulation Leads to Chronic Illness
References
- Turnbaugh PJ et al. The Human Microbiome Project. Nature. 2007
- Belkaid Y & Hand TW. Role of the microbiota in immunity and inflammation. Cell. 2014
- Honda K & Littman DR. The microbiota in adaptive immune homeostasis and disease. Nature. 2016
- Thaiss CA et al. The microbiome and innate immunity. Nature. 2016
- National Institutes of Health. Human Microbiome Research
