How Immune Dysregulation Leads to Chronic Illness
Key takeaways
- Immune dysregulation occurs when the immune system becomes overactive, underactive, or improperly targeted.
- Chronic inflammation is a major consequence of immune imbalance and is linked to many long-term diseases.
- Immune dysregulation can contribute to autoimmune disease, metabolic disorders, and persistent inflammatory conditions.
- Gut health, environmental exposures, stress, and genetics all influence immune system regulation.
- Understanding immune balance helps explain how different chronic illnesses may share similar underlying mechanisms.
However, when immune regulation becomes disrupted, the system can remain overactive, underactive, or misdirected. This state—known as immune dysregulation—can contribute to persistent inflammation and increase the risk of chronic illness.
Scientists increasingly recognize that many long-term health conditions share a common biological feature: an immune system that is no longer properly balanced.
If you want a broader overview of how digestive and immune systems work together, see Digestive and Immune Disorders: How Gut Health Affects the Whole Body.
What Is Immune Dysregulation?
Immune dysregulation refers to a disruption in the normal control mechanisms that regulate immune responses.- Defending against harmful pathogens
- Avoiding unnecessary or excessive immune responses
- Excessive immune activation leading to chronic inflammation
- Misguided immune attacks against healthy tissues (autoimmunity)
- Insufficient immune responses that weaken infection defense
The Role of Inflammation
Inflammation is a natural immune response designed to protect the body during injury or infection.- increase blood flow to the affected area
- recruit immune cells
- initiate tissue repair
However, when immune signaling becomes dysregulated, inflammation can persist even when no immediate threat exists. This condition is often described as chronic low-grade inflammation.
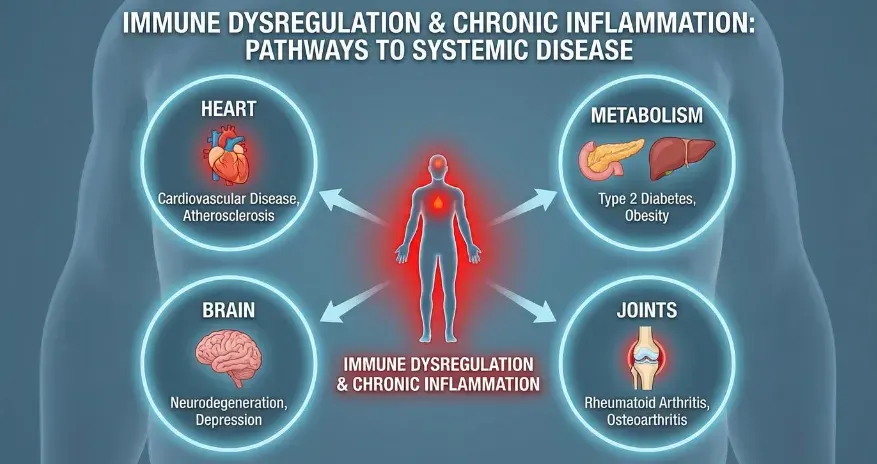
Chronic Illnesses Linked to Immune Dysregulation
Researchers have found that immune imbalance plays a role in many long-term health conditions.Autoimmune Diseases
Autoimmune disorders occur when immune cells attack the body’s own tissues.Examples include:
- rheumatoid arthritis
- lupus
- multiple sclerosis
- Hashimoto’s thyroiditis
Metabolic Diseases
Immune activity also influences metabolism. Chronic inflammation has been associated with conditions such as:- type 2 diabetes
- metabolic syndrome
- fatty liver disease
Cardiovascular Disease
Immune cells play an important role in the development of atherosclerosis, a process in which plaque builds up inside arteries.Neurological Conditions
Inflammation and immune activity are also being studied in relation to neurological conditions such as Alzheimer’s disease, Parkinson’s disease, and multiple sclerosis.How the Gut Influences Immune Regulation
The digestive system contains a large portion of the body’s immune cells. Gut microbes constantly interact with immune tissues in the intestinal lining.- tolerate beneficial microbes
- recognize harmless food particles
- respond appropriately to harmful pathogens
Factors That Can Disrupt Immune Balance
Immune regulation is influenced by many lifestyle, environmental, and biological factors.Chronic Stress
Long-term stress can alter immune signaling through hormonal pathways, potentially increasing inflammatory responses.Poor Sleep
Sleep helps regulate immune function. Sleep deprivation has been associated with increased inflammatory markers.Diet and Nutrition
Nutrient intake and dietary patterns influence immune function, microbial balance, and inflammatory signaling.Environmental Exposures
Pollution, toxins, and other environmental factors may influence immune activity in susceptible individuals.Infections
Certain infections may trigger immune responses that persist beyond the initial illness, potentially contributing to autoimmune or inflammatory conditions.Why Chronic Illness Often Involves Multiple Systems
Many chronic diseases do not affect just one organ. Instead, they involve complex interactions between immune signaling, metabolism, hormonal regulation, and nervous system activity.For example:
- inflammation can affect both joints and cardiovascular health
- immune responses can influence metabolic function
- gut microbes can alter immune and neurological signaling
Supporting Healthy Immune Regulation
Although immune dysregulation involves complex biological mechanisms, several lifestyle factors can support overall immune balance.Balanced Nutrition
Diets rich in fruits, vegetables, whole grains, and diverse plant nutrients support immune function and microbial diversity.Regular Physical Activity
Moderate physical activity can help regulate inflammation and improve metabolic health.Stress Management
Mindfulness practices, relaxation techniques, and psychological support may help reduce chronic stress and improve immune regulation.Sleep Quality
Consistent sleep patterns support immune system recovery and hormonal balance.Medical Care
Individuals with chronic illnesses benefit from appropriate medical diagnosis, monitoring, and treatment.Ongoing Research on Immune Regulation
The science of immune regulation is rapidly evolving. Researchers continue to investigate how genetics, environmental exposures, microbiome changes, and lifestyle factors interact to influence immune function.References
Medzhitov R. “Origin and physiological roles of inflammation.” Nature
Nathan C, Ding A. “Nonresolving inflammation.” Cell
Belkaid Y, Hand TW. “Role of the microbiota in immunity and inflammation.” Cell
National Institutes of Health. Immune System Overview
Hotamisligil GS. “Inflammation and metabolic disorders.” Nature
