Health Conditions Explained: How Diseases Develop and Affect the Body
Health Conditions Explained: How Diseases Develop and Affect the Body
Key takeaways
- Disease typically develops through progressive biological imbalance rather than appearing suddenly.
- Genetic predisposition, environmental exposure, and lifestyle factors interact to influence disease risk.
- Chronic inflammation and cellular dysfunction are common pathways in many long-term conditions.
- Early changes often occur silently before noticeable symptoms develop.
- Understanding disease mechanisms supports prevention and earlier intervention.
Health conditions and diseases are often discussed as isolated problems — heart disease, diabetes, autoimmune disorders, infections — but they all arise from disruptions in how the body normally maintains balance. Understanding how diseases develop provides a clearer framework for prevention, early detection, and long-term health management.
What Is a Health Condition?
A health condition refers to any state that alters normal body structure or function. Conditions may be:
- Acute (short-term, often sudden onset, such as infections or injuries)
- Chronic (long-term and progressive, such as cardiovascular disease or arthritis)
- Genetic (inherited mutations or predispositions)
- Autoimmune (immune system attacking the body’s own tissues)
- Metabolic (disruptions in energy processing and hormone regulation)
How the Body Maintains Balance (Homeostasis)
The human body is designed to maintain homeostasis — a stable internal environment. This includes:
- Stable blood sugar levels
- Regulated blood pressure
- Balanced immune responses
- Proper hormone signaling
- Controlled inflammation
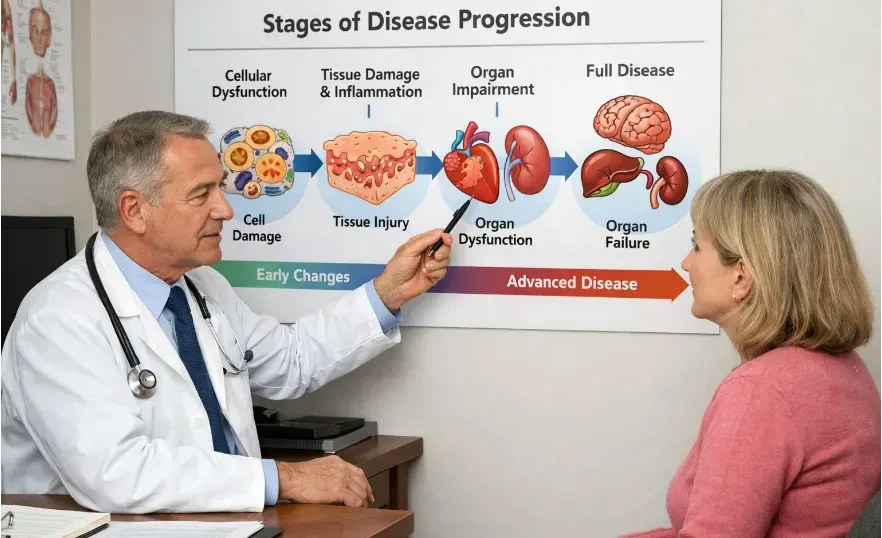
The Stages of Disease Development
Most diseases — particularly chronic ones — follow a recognizable pattern.1. Exposure or Predisposition
This may include:- Genetic susceptibility
- Environmental toxins
- Chronic stress
- Poor nutrition
- Infections
- Sedentary lifestyle
2. Cellular Dysfunction
Cells begin to function inefficiently due to:- Oxidative stress
- Mitochondrial dysfunction
- Persistent inflammation
- Hormonal imbalance
- Impaired immune signaling
3. Tissue and Organ Impact
As cellular damage accumulates:- Blood vessels stiffen
- Joints degrade
- Insulin signaling weakens
- Immune regulation becomes unstable
- Organs begin compensating under stress
4. Clinical Disease
When structural or functional disruption crosses a threshold, diagnosable disease is identified. Examples include:- Type 2 diabetes
- Coronary artery disease
- Autoimmune disorders
- Chronic kidney disease
Acute vs. Chronic Disease: Key Differences
| Feature | Acute Disease | Chronic Disease |
|---|---|---|
| Onset | Rapid | Gradual |
| Duration | Short-term | Long-term |
| Cause | Often infection or injury | Multifactorial |
| Progression | Self-limited or treated | Progressive without intervention |
| Examples | Flu, appendicitis | Diabetes, hypertension |
Acute disease typically results from a clear trigger. Chronic disease develops through prolonged imbalance and cumulative exposure.
Common Biological Pathways Behind Many Diseases
Although diseases appear different on the surface, many share overlapping biological mechanisms.Chronic Inflammation
Persistent low-grade inflammation is linked to cardiovascular disease, metabolic syndrome, autoimmune disorders, neurodegenerative disease, and certain cancers.Oxidative Stress
An imbalance between free radicals and antioxidant defenses damages cellular structures, DNA, and proteins.Insulin Resistance
A key mechanism in metabolic disorders, insulin resistance contributes to obesity-related conditions, cardiovascular disease, and type 2 diabetes.Immune Dysregulation
An overactive or underactive immune system increases vulnerability to infection, autoimmunity, and chronic inflammatory disease.Why Symptoms Often Appear Late
Many chronic diseases develop silently over years. The body compensates effectively — until it cannot.- Blood sugar may remain normal while insulin levels rise.
- Blood pressure may creep upward without symptoms.
- Arteries may narrow before chest pain occurs.
The Role of Genetics vs. Environment
Genetics load the gun; environment pulls the trigger. While some diseases are strongly inherited, most common chronic diseases arise from an interaction between:- Genetic predisposition
- Diet and physical activity
- Sleep quality
- Stress exposure
- Environmental toxins
- Social determinants of health
Can Disease Be Reversed?
The answer depends on the stage and condition.- Early metabolic dysfunction can sometimes be reversed.
- Structural damage (e.g., advanced atherosclerosis) may be slowed but not fully reversed.
- Autoimmune conditions can often be managed into remission.
- Some infectious diseases are fully curable.
A Framework for Understanding Health
Instead of viewing disease as isolated diagnoses, it can be helpful to think in layers:- Lifestyle and environment
- Biological processes
- Organ system function
- Clinical symptoms
- Diagnosed disease
Articles in This Pillar
To explore specific aspects of disease development in more depth, continue with:- What Causes Chronic Disease? Genetics, Lifestyle, and Environment
- Inflammation: The Common Link Between Many Diseases
- Can Most Chronic Diseases Be Prevented?
- Early Warning Signs Your Body Is Out of Balance
References
- World Health Organization (WHO). Noncommunicable diseases: Key facts and global burden data
- Centers for Disease Control and Prevention (CDC). Chronic Disease Overview and Prevention Strategies
- National Institutes of Health (NIH). Inflammation and its role in health and disease
- Institute of Medicine. The Future of Public Health
- Harvard T.H. Chan School of Public Health. The interplay of genetics and lifestyle in chronic disease risk
