What Causes Chronic Disease? Genetics, Lifestyle, and Environment
Key takeaways
- Most chronic diseases result from multiple interacting causes rather than one single trigger.
- Genetics influences susceptibility, but lifestyle and environment often determine how risk expresses over time.
- Common pathways include inflammation, metabolic dysfunction, and cumulative cellular stress.
- Small, repeated exposures (diet, sleep loss, stress, pollutants) can add up to major long-term impact.
- Reducing modifiable risks can meaningfully lower disease likelihood even with a family history.
Chronic disease rarely comes from a single cause. Most long-term conditions develop when genetics, lifestyle, and environmental exposures interact over time—shifting the body away from stability and toward ongoing dysfunction. If you want the big-picture framework for how disease develops in the body, start with Health Conditions Explained: How Diseases Develop and Affect the Body.
The key idea is this: risk is cumulative. Your genes may raise or lower your baseline vulnerability, but day-to-day exposures and behaviors often influence whether that risk becomes an actual diagnosis.
What Counts as a Chronic Disease?
A chronic disease is typically defined by long duration and slow progression, often requiring ongoing management. Common examples include:
- Cardiovascular disease (e.g., coronary artery disease, hypertension)
- Type 2 diabetes
- Chronic respiratory diseases (e.g., COPD, asthma)
- Certain cancers
- Autoimmune and inflammatory conditions (e.g., rheumatoid arthritis, inflammatory bowel disease)
- Chronic kidney disease
Not every chronic condition is preventable, but many are influenced by modifiable risk factors—especially those linked to metabolism, inflammation, and long-term stress load.
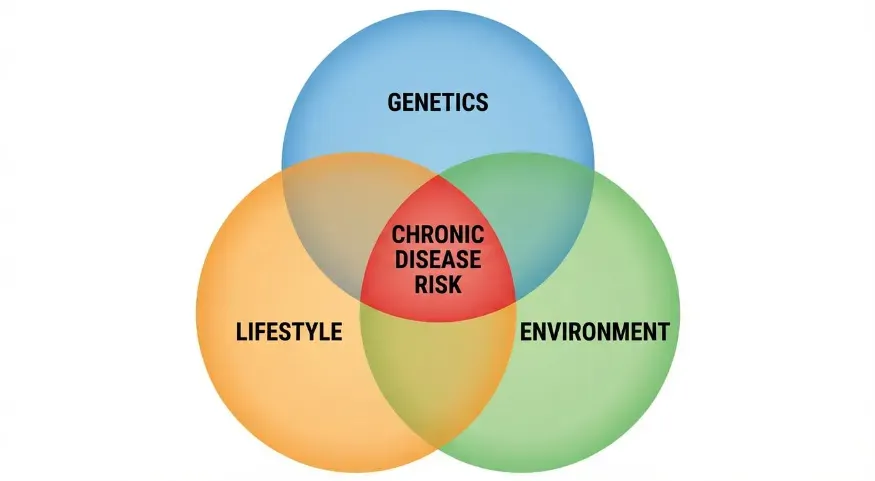
The “Three-Lens” Model: Genes, Lifestyle, Environment
A helpful way to understand chronic disease causation is to view risk through three lenses:- Genetic susceptibility (what you inherit)
- Lifestyle exposures (what you repeatedly do)
- Environmental context (what you repeatedly encounter)
Chronic disease often develops when multiple lenses align in the wrong direction for long enough.
Genetics: Predisposition Is Not Destiny
What genetics can do
Genes can influence:- How you process fats and sugars
- How strongly you mount inflammatory responses
- How you handle oxidative stress
- How your blood pressure and cholesterol tend to run
- How your immune system distinguishes “self” from “non-self”
Some conditions have strong genetic drivers. Others reflect genetic tendencies that need environmental or lifestyle “push” to become disease.
Family history vs. single-gene disorders
It helps to separate two concepts:- Single-gene disorders (rare): One mutation strongly predicts disease.
- Polygenic risk (common): Many small genetic differences collectively raise risk.
Most widespread chronic diseases—like type 2 diabetes and heart disease—are generally polygenic and heavily shaped by non-genetic factors.
Epigenetics: how exposures influence gene expression
Epigenetics describes changes that affect how genes are turned on or off (without changing the DNA sequence). Over time, patterns of:- diet quality
- sleep
- stress
- physical activity
- toxin exposure
Lifestyle: Daily Inputs That Build Long-Term Outcomes
Lifestyle factors often work through predictable biological pathways: insulin signaling, blood pressure regulation, immune tone, and repair capacity.Nutrition patterns
Chronic disease risk is influenced less by single foods and more by repeated patterns, such as:- Excess ultra-processed foods and added sugars
- Low fiber intake
- Imbalanced fats (especially high trans fats)
- Low micronutrient density
- Excess overall energy intake relative to needs
Over time, poor nutrition can contribute to insulin resistance, dyslipidemia, chronic inflammation, and fatty liver changes, which are core drivers of many chronic conditions.
Physical activity and sedentary time
Movement affects:- glucose uptake by muscles
- blood vessel function
- inflammation regulation
- body composition
- blood pressure
Sleep and circadian disruption
Short sleep and irregular schedules can influence:- appetite hormones and food cravings
- insulin sensitivity
- stress hormone patterns
- immune regulation
Chronic stress and coping capacity
Stress isn’t only “in your head.” Long-term stress can alter:- cortisol and autonomic nervous system tone
- inflammation signaling
- blood pressure patterns
- sleep quality
- health behaviors (food, alcohol, activity)
Stress often acts as a risk amplifier, making other factors (diet, sleep, inflammation) harder to control.
Substance exposures
Long-term risk is affected by:- tobacco exposure (active or secondhand)
- heavy or chronic alcohol use
- certain drug exposures (including misuse of prescribed substances)
Environment: The Risk Factors Around You
Environment is broader than air quality. It includes physical exposures, social context, and access to resources that shape health behaviors.Physical environment
Examples include:- Air pollution exposure
- Occupational exposures (dusts, chemicals, fumes)
- Water contaminants
- Built environment (walkability, safety, green space)
Food environment and access
Where you live strongly affects what’s easy to eat. A “healthy choice” becomes harder when someone’s environment consistently pushes:- low-cost, calorie-dense foods
- limited fresh produce
- long work hours and commuting time
- limited cooking facilities or time
Social determinants of health
Long-term chronic disease patterns are strongly shaped by:- income stability
- education access
- housing stability
- discrimination and chronic stress burden
- access to preventive healthcare
How These Factors Combine in the Body
Even though chronic diseases look different, many share core internal processes.Metabolic dysfunction
Repeated overnutrition, inactivity, sleep loss, and stress can push the body toward:- insulin resistance
- higher triglycerides
- lower HDL cholesterol
- higher blood pressure
- abdominal fat accumulation
Chronic inflammation
Persistent inflammatory signaling can come from:- excess visceral fat
- poor sleep
- chronic stress
- exposure to pollutants
- untreated infections or autoimmune processes
Cumulative cellular stress and impaired repair
When exposure load exceeds repair capacity, the body can shift into a state of:- oxidative stress
- mitochondrial dysfunction
- impaired tissue regeneration
Why Two People With Similar Habits Can Have Different Outcomes
It’s common to see variability: one person develops diabetes, another doesn’t—despite similar lifestyles. Reasons may include:- different genetic susceptibility
- different early-life exposures
- differences in sleep, stress, and daily movement
- differences in muscle mass and body fat distribution
- differences in access to healthcare and early intervention
- differences in environmental exposures (air quality, work hazards)
This is why chronic disease is best understood as risk gradients, not a simple “healthy vs. unhealthy” binary.
What You Can Control: A Practical Prevention Lens
Even when you can’t change genetics or every exposure, many leverage points are modifiable:- Improve diet pattern quality (especially fiber and minimally processed foods)
- Increase weekly movement and reduce sedentary time
- Normalize sleep duration and consistency
- Build stress management routines you can sustain
- Avoid tobacco exposure and limit high-risk substance use
- Use preventive care and screenings to catch early shifts
Chronic disease prevention is rarely about perfection. It’s more often about consistent, high-yield changes that reduce exposure load and improve regulation.
When to Seek Medical Guidance
If you have any of the following, it’s worth discussing risk with a clinician:- strong family history of early cardiovascular disease, diabetes, or autoimmune disease
- persistent high blood pressure, high blood sugar, or abnormal lipids
- symptoms that persist (fatigue, unexplained weight changes, frequent infections, chronic pain)
- major lifestyle changes that aren’t improving biomarkers over time
References
- World Health Organization (WHO). Noncommunicable diseases (NCDs): burden, risk factors, and prevention overview.
- Centers for Disease Control and Prevention (CDC). Chronic disease prevention and health promotion resources.
- National Institutes of Health (NIH). Genetics and complex disease risk; gene–environment interactions.
- American Heart Association (AHA). Lifestyle and risk factor guidance for cardiovascular disease prevention.
- National Institute of Environmental Health Sciences (NIEHS). Environmental exposures and chronic disease risk.
