Living With Chronic Conditions: Management, Adaptation, and Quality of Life
Living With Chronic Conditions: Management, Adaptation, and Quality of Life
Key takeaways
- Chronic conditions often require ongoing management rather than one-time treatment.
- Effective disease management combines medical care, lifestyle adjustments, and regular monitoring.
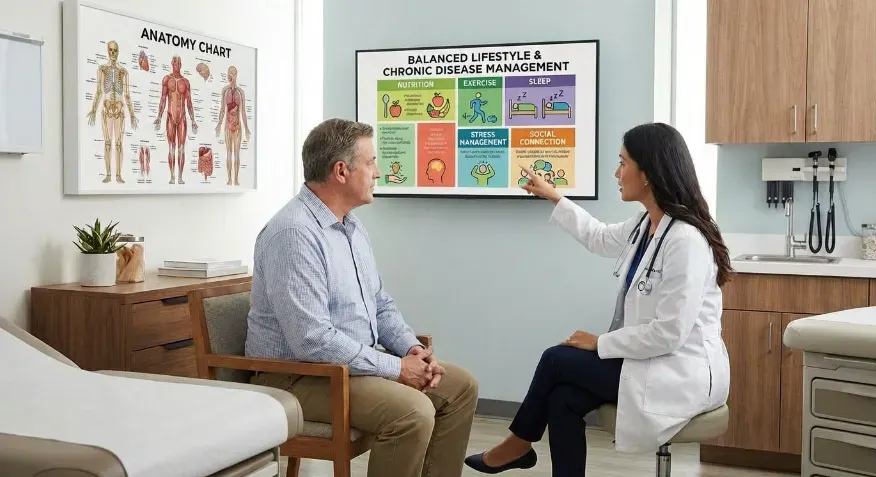
- Daily habits such as nutrition, physical activity, and sleep can significantly influence long-term outcomes.
- Tracking symptoms and health metrics helps individuals and clinicians adjust treatment plans.
- Psychological adaptation and social support are essential components of long-term quality of life.
What Is a Chronic Condition?
A chronic condition is a health condition that typically lasts a year or longer and often requires ongoing medical attention or lifestyle management. Unlike acute illnesses, which resolve quickly, chronic diseases usually develop gradually and persist over time.
- Diabetes
- Heart disease
- Asthma
- Arthritis
- Chronic kidney disease
- Autoimmune disorders
- Chronic respiratory diseases
The Core Principles of Chronic Disease Management
Managing a chronic illness involves more than simply taking medication. Effective long-term management typically includes several interconnected strategies.Medical Treatment and Care Plans
Most chronic conditions require ongoing medical care guided by healthcare professionals. Treatment plans may include:
- Prescription medications
- Regular medical appointments
- Diagnostic tests or screenings
- Physical therapy or rehabilitation
- Specialist consultations
Lifestyle Adaptation
Daily habits play a major role in disease management. Lifestyle adjustments can help reduce symptoms, lower complications, and improve overall health. Common areas of focus include:- Balanced nutrition
- Regular physical activity
- Adequate sleep
- Stress management
- Avoidance of harmful habits such as smoking
Symptom and Health Monitoring
Tracking health metrics allows individuals and healthcare providers to detect changes early.- Blood glucose measurements
- Blood pressure tracking
- Weight changes
- Symptom journals
- Wearable health device data
Long-Term Prevention
Many chronic diseases are linked to complications that develop over time. Prevention strategies often focus on:
- Early detection of disease progression
- Managing risk factors
- Preventing hospitalizations
- Maintaining mobility and independence
Adapting to Life With a Chronic Illness
A chronic diagnosis often requires adjustments beyond physical health. People frequently need to adapt routines, expectations, and coping strategies.Building Sustainable Routines
Consistency is often more effective than extreme changes. Sustainable routines may include:- Structured medication schedules
- Planned meal patterns
- Regular exercise adapted to ability
- Predictable sleep schedules
Managing Emotional and Psychological Impact
Chronic illness can affect mental health. People may experience:- Stress or anxiety about symptoms
- Frustration with physical limitations
- Fatigue from ongoing care routines
- Social isolation
- Counseling or therapy
- Support groups
- Stress reduction techniques
- Mindfulness or relaxation practices
Maintaining Independence and Function
One goal of chronic care is preserving daily functioning and independence. This may involve:
- Physical therapy
- Assistive devices
- Occupational therapy
- Home adaptations
- Energy management techniques
The Role of Self-Management Skills
People living with chronic conditions often become active participants in their own healthcare. Self-management skills help individuals make informed decisions and respond to changes in their condition.- Understanding medications and treatments
- Recognizing symptom changes
- Communicating effectively with healthcare providers
- Setting realistic health goals
- Making informed lifestyle decisions
How Healthcare Teams Support Chronic Care
Managing long-term illness is usually a collaborative process involving multiple professionals.- Primary care physicians
- Medical specialists
- Nurses
- Dietitians
- Physical therapists
- Mental health professionals
Long-Term Quality of Life With Chronic Disease
Quality of life is an important outcome in chronic disease management. Even when symptoms cannot be completely eliminated, many individuals maintain meaningful lives through effective management strategies.- Stable symptom control
- Functional independence
- Supportive relationships
- Access to healthcare
- Personal coping strategies
