Depression: Biological and Lifestyle Factors
Key takeaways
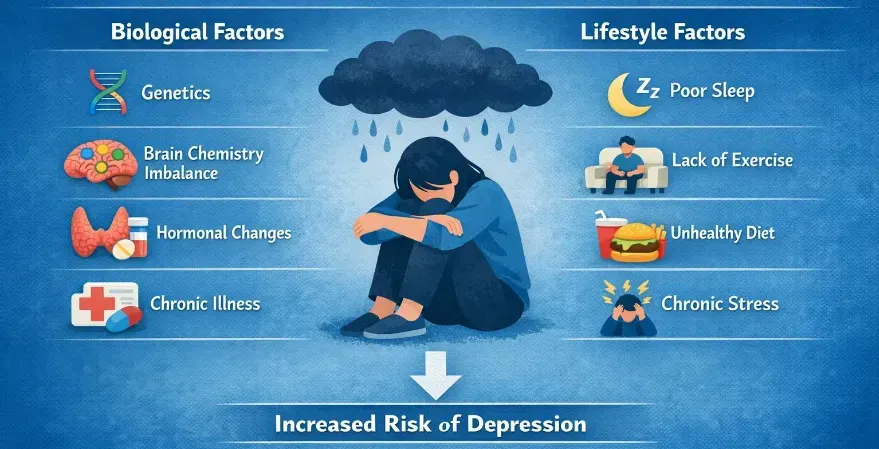
- Depression is influenced by multiple factors including brain chemistry, genetics, hormones, and environmental stress.
- Neurotransmitters such as serotonin, dopamine, and norepinephrine play important roles in mood regulation.
- Hormonal systems, particularly stress hormones, can influence emotional resilience and mental health.
- Lifestyle factors such as sleep, nutrition, physical activity, and social support significantly affect depression risk.
- Early recognition and comprehensive treatment can improve outcomes and long-term well-being.
Research shows that depression develops through a combination of biological, psychological, and lifestyle factors. Changes in brain chemistry, hormonal regulation, and neural signaling often interact with life stress, sleep patterns, physical health, and environmental influences.
To understand how these biological systems interact with mood and mental health, it is helpful to explore the broader relationship between brain signaling and hormone regulation discussed in Neurological and Hormonal Conditions: Brain, Mood, and Balance.
What Is Depression?
Depression, also known as major depressive disorder, is a mental health condition characterized by persistent sadness, loss of interest in activities, and reduced motivation. Symptoms typically last for weeks or longer and may vary in severity.
- emotional well-being
- cognitive functioning
- physical health
- daily productivity
- interpersonal relationships
Biological Factors in Depression
Scientific research increasingly highlights the role of biological processes in depression. Changes in brain chemistry, neural connectivity, and hormone regulation can influence mood and emotional stability.Neurotransmitter Imbalances
Neurotransmitters are chemical messengers that allow brain cells to communicate with one another. Several neurotransmitters are involved in mood regulation.- Serotonin, which helps regulate mood, sleep, and appetite
- Dopamine, involved in motivation and reward processing
- Norepinephrine, which influences alertness and stress responses
Brain Structure and Neural Circuits
Neuroimaging studies have identified differences in certain brain regions among individuals experiencing depression. Areas involved in emotional processing and decision-making may show altered activity.- the prefrontal cortex, which helps regulate emotions and decision-making
- the amygdala, involved in processing emotional responses
- the hippocampus, associated with memory and stress regulation
Hormonal and Stress System Dysregulation
The body’s stress response system, particularly the hypothalamic–pituitary–adrenal (HPA) axis, plays a role in depression.
Hormonal changes associated with life stages such as pregnancy, postpartum periods, and menopause may also influence vulnerability to depression.
Genetic Influences
Genetics can contribute to the likelihood of developing depression. Individuals with a family history of depression or other mood disorders may have a higher risk.Lifestyle Factors That Influence Depression
While biological factors play a significant role, lifestyle patterns and environmental conditions also strongly influence mental health.Chronic Stress
Prolonged stress can disrupt hormonal balance and alter neural circuits involved in emotional regulation. Work stress, financial concerns, relationship challenges, or major life transitions may contribute to depressive symptoms.Sleep Disruption
Sleep and mood are closely connected. Poor sleep quality or chronic sleep deprivation can affect neurotransmitter balance and stress hormone regulation.- insomnia
- difficulty staying asleep
- excessive sleep or fatigue
Physical Activity and Brain Health
Regular physical activity supports brain health through several mechanisms. Exercise can help:
- stimulate neurotransmitter production
- reduce stress hormone levels
- improve sleep quality
- support cognitive function
Nutrition and Metabolic Health
Diet influences brain function and mental health. Nutrient deficiencies or metabolic imbalance may affect neurotransmitter production and brain signaling.Nutrients linked to brain health include:
- omega-3 fatty acids
- B vitamins
- magnesium
- amino acids used in neurotransmitter synthesis
Social Support and Environment
Social relationships and community support play important roles in mental well-being. Isolation, loneliness, or lack of support networks can increase vulnerability to depression.Recognizing Symptoms of Depression
Depression symptoms can vary between individuals but often include a combination of emotional, cognitive, and physical changes.Common symptoms include:
- persistent sadness or low mood
- loss of interest in previously enjoyable activities
- fatigue or low energy
- difficulty concentrating
- changes in appetite or weight
- sleep disturbances
- feelings of worthlessness or guilt
Treatment and Management Approaches
Depression is treatable, and many individuals improve with appropriate care and support. Effective treatment often combines multiple strategies.Psychological Therapies
Psychological therapies help individuals understand thought patterns and develop coping strategies.- cognitive behavioral therapy (CBT)
- interpersonal therapy
- behavioral activation strategies
Medical Treatments
Healthcare providers may recommend medication to help regulate neurotransmitter activity.- selective serotonin reuptake inhibitors (SSRIs)
- serotonin-norepinephrine reuptake inhibitors (SNRIs)
- other antidepressant medications depending on individual needs
Lifestyle and Preventive Strategies
Lifestyle adjustments can complement clinical treatments and support long-term mental health.- maintaining regular sleep routines
- engaging in physical activity
- practicing stress-management techniques
- building supportive relationships
- seeking counseling or peer support when needed
Long-Term Outlook
Depression is a multifaceted condition influenced by both biological and environmental factors. Understanding the interaction between brain chemistry, hormones, lifestyle, and life experiences helps guide effective prevention and treatment strategies.References
- National Institute of Mental Health (NIMH). Major Depression
- World Health Organization (WHO). Depression and Other Common Mental Disorders: Global Health Estimates
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders (DSM-5)
- Harvard Medical School. Understanding the Neurobiology of Depression
- National Institute of Neurological Disorders and Stroke (NINDS). Brain Basics: Mood Disorders
