Key takeaways
- The prostate’s position means urinary and reproductive functions are closely linked.
- Prostatitis, BPH, and cancer are the most common prostate conditions—symptoms can overlap.
- Age-related changes make prostate issues common, but they are treatable when addressed early.
Understanding the Prostate: What It Is and What It Does
The prostate is a small exocrine gland in men that plays a dual role: it’s part of the reproductive system and it interacts directly with the urinary tract. Located just below the bladder, the prostate surrounds the first portion of the urethra—the tube that carries urine from the bladder to the outside of the body. Its primary reproductive job is to produce 50–60% of the fluid that makes up semen. This fluid nourishes and transports sperm, contributing to fertility in humans as in all mammals.
Because the urethra passes directly through it, the prostate’s health directly affects urination. This “strategic” location makes the gland a central player—the nexus—of both reproductive and urinary systems. Any changes in size, shape, or tissue structure—whether from infection, benign growth, or cancer—can cause symptoms in either or both systems. Understanding this shared pipeline is key to making sense of the common conditions men face.
Prostatitis: When the Gland Feels Inflamed
Prostatitis is inflammation of the prostate gland, and in younger men it’s often the most common prostate-related diagnosis. The inflammation may be due to bacterial infection, but not always—many cases are nonbacterial prostatitis or chronic pelvic pain syndrome. When infection is present, it can be bacterial (acute or chronic) or occasionally viral. Symptoms often include pelvic discomfort, pain during urination or ejaculation, increased urinary frequency, and sometimes fever or malaise.
Chronic prostatitis can be particularly frustrating. Even after treating a bacterial infection, some men have lingering pelvic pain or urinary symptoms due to inflammation or nerve hypersensitivity. Management can include antibiotics, anti-inflammatory medication, pelvic floor physical therapy, and lifestyle adjustments. The condition can significantly affect quality of life, so early evaluation and tailored care are essential.
Benign Prostatic Hyperplasia (BPH): Enlargement and Urinary Impact
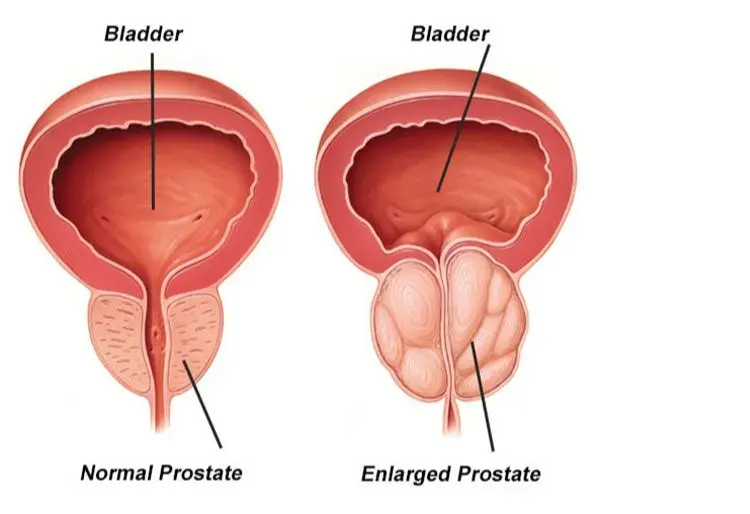
As men age, the prostate undergoes a second growth phase, beginning subtly in midlife. This noncancerous enlargement—benign prostatic hyperplasia (BPH)—is one of the most common causes of urinary symptoms in men over 50. The growth usually occurs in the central (transition) zone of the prostate, which surrounds the urethra. As the gland expands, it squeezes this channel, creating resistance to urine flow.
This narrowing forces the bladder muscle to contract harder, which over time can lead to changes in the bladder wall. It may become thicker, less elastic, and less able to store urine comfortably—reducing capacity and triggering more frequent urges. The result is a cluster of symptoms collectively called lower urinary tract symptoms (LUTS), including weak stream, difficulty starting urination, dribbling at the end, urgency, and increased frequency—especially at night.
How BPH Leads to Lower Urinary Tract Symptoms (LUTS)
Think of the urethra like a garden hose and the prostate like a hand squeezing it. As the squeeze increases, the water (urine) struggles to flow through. The bladder, like a pump, has to work harder against the resistance. Over time, the “pump” muscle may tire, leading to incomplete emptying and more frequent trips to the bathroom. In severe cases, obstruction can cause acute urinary retention—a sudden inability to urinate.
The changes aren’t just mechanical; they affect bladder behavior. A bladder that’s used to high pressure can become irritable, contracting before it’s full. That’s why some men with BPH feel an urgent need to go even when their bladder volume is low. Addressing BPH early can prevent or slow these changes.
How Common Is BPH—And Who Experiences It?
BPH prevalence rises sharply with age. Around 50–60% of men in their 50s have some lower urinary tract dysfunction, and by their 60s that number climbs to 75–80%. Some global studies estimate that about 94 million men live with BPH at any given time. In some populations, moderate to severe LUTS are seen in over half of men by their 80s.
These statistics make BPH almost an expected part of male aging—but “common” doesn’t mean “harmless.” Untreated obstruction can cause bladder damage, kidney strain, and recurring urinary tract infections. Men often delay seeking care, chalking symptoms up to aging, but evaluation can open options from lifestyle adjustments to medications or minimally invasive procedures.
Prostate Cancer: A Different Set of Risks
Prostate cancer is a malignant growth within the gland, and it’s the second most commonly diagnosed cancer in men worldwide. Each year, about 1.2 million new cases are diagnosed, and one in eight men will face it in their lifetime. The average age at diagnosis is 67, though some cases appear earlier, especially with certain genetic risks such as BRCA2 mutations.
Unlike BPH, which grows inward and squeezes the urethra, prostate cancer often develops in the peripheral zone of the gland, where it may not initially cause urinary symptoms. This means cancer can remain silent until it’s more advanced, making screening—through PSA blood tests and digital rectal exams—an important tool for early detection.
How Common Is Prostate Cancer and When to Investigate
While prostate cancer can be slow-growing, aggressive types do occur, and early identification matters. Men with family history, African ancestry, or certain genetic profiles may face higher risks. Warning signs—when they appear—can mimic BPH symptoms: hesitancy, weak stream, or frequent urination. Blood in urine or semen, bone pain, and unexplained weight loss are later signs.
Because symptoms overlap, men over 50 (or earlier with risk factors) should discuss PSA testing with their doctor. Even when cancer isn’t present, the process helps detect BPH and other treatable conditions before they cause complications.
When to See a Doctor—Know the Red Flags
Many men normalize urinary symptoms as “just getting older,” but certain changes should prompt medical attention. These include sudden urinary retention, visible blood in urine or semen, persistent pelvic or lower back pain, or a rapid worsening of urinary symptoms.
The good news is that most prostate problems—including BPH and prostatitis—are treatable, and early management can preserve urinary function and quality of life. Whether it’s medication, procedural therapy, or simply monitoring, there’s no reason to suffer in silence.
Supporting Citations

